Presenting Boppli®
Accurate1, non-invasive, continuous, wireless BP monitoring for neonatal patients.
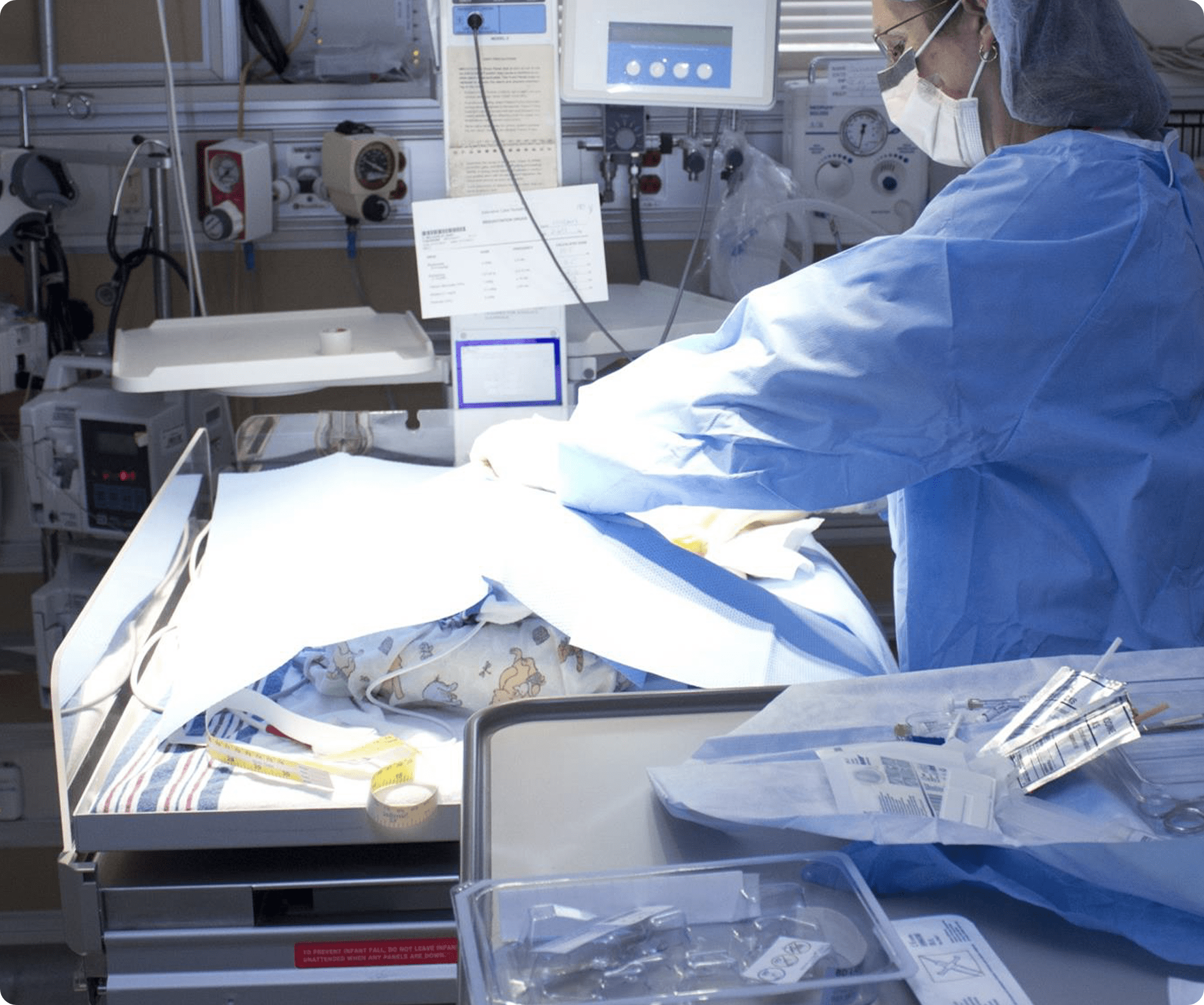
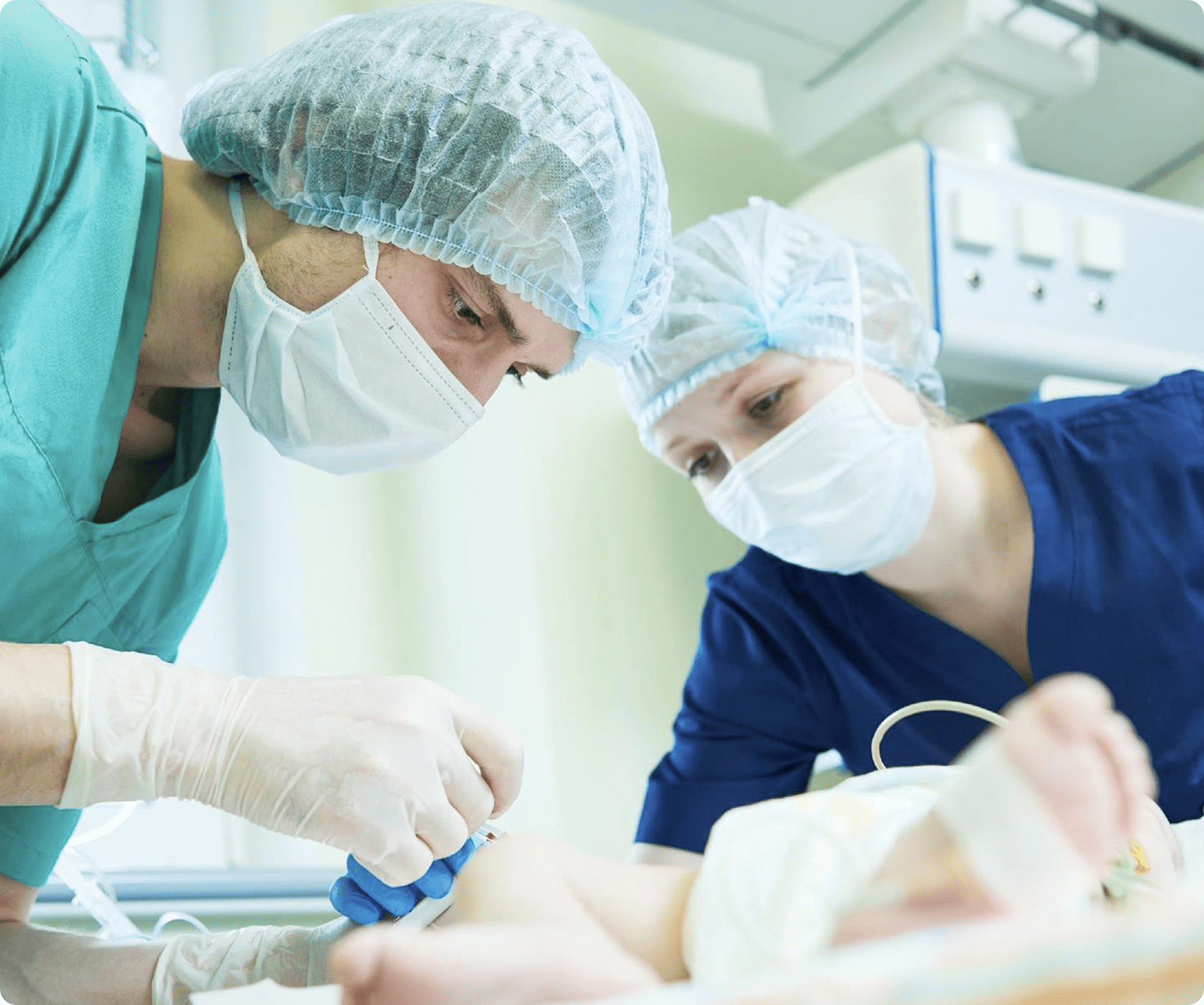
Boppli is a highly-advanced non-invasive blood pressure monitoring device that is ideal for fragile neonatal infants in the NICU. It provides an option for moderately and mildly sick patients who require continuous blood pressure measurements, without the potential complications of an arterial line.
Boppli has the potential to revolutionize the standard of care for continuous blood pressure monitoring for neonates. Our technology is safer than an arterial line. It’s non-invasive, painless, wireless, and silent.
2020 FDA Breakthrough Device Designation
2020 SWPDC Pediatric Device Award
2019 Winner of the NCC Pediatric Device Pitch Competition
2020 NCC-PDI MedTech Innovator Pediatric Accelerator
Our NICU Platform:
The Boppli® Band Wearable Sensor
+